What Causes Plantar Warts?
 Warts, which can grow throughout the body, are outgrowths on the skin that are caused by human papillomavirus (HPV). Warts can be very contagious, and they can spread through skin-to-skin contact or through sharing personal items. Plantar warts grow on the bottom of the feet and usually have tiny black dots in them. Generally, warts disappear over time, but it may take months for them to do so. While plantar warts are usually harmless, they can be very painful. There are a variety of treatment options for warts that are causing pain, including chemical treatments and lasers. Some podiatrists may even elect to surgically remove warts that have become a problem. If you are experiencing painful plantar warts, make sure to discuss with a podiatrist which treatment options may be right for you.
Warts, which can grow throughout the body, are outgrowths on the skin that are caused by human papillomavirus (HPV). Warts can be very contagious, and they can spread through skin-to-skin contact or through sharing personal items. Plantar warts grow on the bottom of the feet and usually have tiny black dots in them. Generally, warts disappear over time, but it may take months for them to do so. While plantar warts are usually harmless, they can be very painful. There are a variety of treatment options for warts that are causing pain, including chemical treatments and lasers. Some podiatrists may even elect to surgically remove warts that have become a problem. If you are experiencing painful plantar warts, make sure to discuss with a podiatrist which treatment options may be right for you.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Scott Peters from Ankle & Foot Walk-In Clinic. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in Mayfield Village, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
All About Plantar Warts
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.
What is a Bunion?
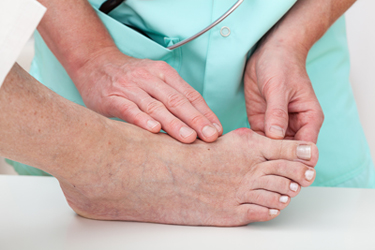 The medical term for a bunion is referred to as hallux valgus. It appears as a bony protrusion that forms on the side of the big toe and may cause wearing shoes to be uncomfortable. The big toe can become misaligned, and may affect the remaining toes. Some of the symptoms that are associated with this condition can include pain, inflammation, and the toe may appear red. If a bunion is left untreated, arthritis may develop, which can cause deeper joint pain. Genetic factors may play a significant role in developing a bunion, in addition to wearing shoes that do not have ample room for the toes to move freely in. If you notice a bump extending from your toe, it is suggested that you consult with a podiatrist who can properly diagnose and treat bunions.
The medical term for a bunion is referred to as hallux valgus. It appears as a bony protrusion that forms on the side of the big toe and may cause wearing shoes to be uncomfortable. The big toe can become misaligned, and may affect the remaining toes. Some of the symptoms that are associated with this condition can include pain, inflammation, and the toe may appear red. If a bunion is left untreated, arthritis may develop, which can cause deeper joint pain. Genetic factors may play a significant role in developing a bunion, in addition to wearing shoes that do not have ample room for the toes to move freely in. If you notice a bump extending from your toe, it is suggested that you consult with a podiatrist who can properly diagnose and treat bunions.
If you are suffering from bunions, contact Dr. Scott Peters of Ankle & Foot Walk-In Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our office located in Mayfield Village, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
My Teenager and Sever’s Disease
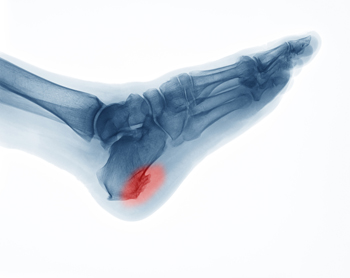 The age group of people who are typically affected by Sever’s disease is between ten and fourteen. It impacts the growth plate in the heel and can cause severe pain and discomfort. It can happen as a result of participating in running and jumping activities, which can exert excess pressure on the heel. It is beneficial to perform stretches that can loosen the Achilles tendon which is connected to the heel. Additionally, many patients wear specific types of footwear that can help in the healing process. If you notice your child is limping or complaining of heel pain, it is strongly suggested that you schedule an appointment with a podiatrist who can diagnose and treat Sever’s disease.
The age group of people who are typically affected by Sever’s disease is between ten and fourteen. It impacts the growth plate in the heel and can cause severe pain and discomfort. It can happen as a result of participating in running and jumping activities, which can exert excess pressure on the heel. It is beneficial to perform stretches that can loosen the Achilles tendon which is connected to the heel. Additionally, many patients wear specific types of footwear that can help in the healing process. If you notice your child is limping or complaining of heel pain, it is strongly suggested that you schedule an appointment with a podiatrist who can diagnose and treat Sever’s disease.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see Dr. Scott Peters from Ankle & Foot Walk-In Clinic. Our doctor can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact our office located in Mayfield Village, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle injuries.
Sever's Disease
Sever’s disease, also known as calcaneal apophysitis is a common bone disorder that occurs during childhood. The disease is defined as an inflammation of the growth plate in the heel. When a child has a growth spurt, his heel bone grows faster than the muscles, tendons, and ligaments in his leg. This disease is a result of overuse. The people who are most likely to be affected by this disease are children who are in a growth spurt, especially boys who are from the ages of 5 to 13 years old. 60% of children with Sever’s disease have both heels involved.
Symptoms of this disease are heel pain that intensifies during running and jumping activities. The pain is typically localized to the posterior part of the heel. Symptoms may be severe, and they can easily interfere with daily activities. Children who play soccer, baseball, and basketball are more likely to develop Sever’s disease.
Your doctor will diagnose your child based on his or her symptoms, x-rays are generally not helpful in diagnosing this disease. Your doctor may examine both heels and ask your child questions about his or her activity level in sports. Your doctor may then use the squeeze test on your child’s heel to see if there is any pain. Nevertheless, some doctors might still use x-rays to rule out any other issues such as fractures, infections, and tumors.
Sever’s disease can be prevented by maintaining good flexibility while your child is growing. Another prevention method is to wear good-quality shoes that have firm support and a shock-absorbent sole. Sever’s disease can be treated by ceasing any activity that causes heel pain. You should apply ice to the injured heel for 20 minutes 3 times a day. Additionally, orthotics should be used for children who have high arches, flat feet, or bowed legs.
If you suspect your child has Sever’s disease, you should make an appointment with your podiatrist to have his or her foot examined. Your doctor may recommend nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen to relieve pain. In more severe cases, your child may need a cast to rest his or her heel. Fortunately, Sever’s disease does not cause long-term foot problems. After treatment, your child should start to feel better within two weeks to two months.
Caring for Foot Wounds
 Our feet endure pressure during the majority of the day. It is important to promptly treat existing cuts or bruises on the feet, as this may be helpful in preventing foot wounds from developing. Patients who may be susceptible to developing wounds on the feet can include people who are diabetic or have medical conditions consisting of elevated cholesterol and blood pressure. It is beneficial to wear shoes and socks that are comfortable, in addition to trimming the toenails properly. A wound on the foot will heal faster when treated quickly, and it is strongly advised that you speak with a podiatrist who can effectively treat foot wounds.
Our feet endure pressure during the majority of the day. It is important to promptly treat existing cuts or bruises on the feet, as this may be helpful in preventing foot wounds from developing. Patients who may be susceptible to developing wounds on the feet can include people who are diabetic or have medical conditions consisting of elevated cholesterol and blood pressure. It is beneficial to wear shoes and socks that are comfortable, in addition to trimming the toenails properly. A wound on the foot will heal faster when treated quickly, and it is strongly advised that you speak with a podiatrist who can effectively treat foot wounds.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Scott Peters from Ankle & Foot Walk-In Clinic. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Mayfield Village, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Neuropathy
Neuropathy is a condition in which the nerves in the body become damaged from a number of different illnesses. Nerves from any part of the body, including the foot, can be damaged. There are several forms of neuropathy including peripheral neuropathy, cranial neuropathy, focal neuropathy, and autonomic neuropathy. Furthermore there is also mononeuropathy and polyneuropathy. Mononeuropathies affect one nerve while polyneuropathies affect several nerves. Causes of neuropathy include physical injury, diseases, cancers, infections, diabetes, toxic substances, and disorders. It is peripheral neuropathy that affects the feet.
The symptoms of neuropathy vary greatly and can be minor such as numbness, sensation loss, prickling, and tingling sensations. More painful symptoms include throbbing, burning, freezing, and sharp pains. The most severe symptoms can be muscle weakness/paralysis, problems with coordination, and falling.
Podiatrists rely upon a full medical history and a neurological examination to diagnose peripheral neuropathy in the foot. More tests that may be used include nerve function tests to test nerve damage, blood tests to detect diabetes or vitamin deficiencies. Imaging tests, such as CT or MRI scans, might be used to look for abnormalities, and finally nerve or skin biopsies could also be taken.
Treatment depends upon the causes of neuropathy. If the neuropathy was caused by vitamin deficiency, diabetes, infection, or toxic substances, addressing those conditions can lead to the nerve healing and sensation returning to the area. However if the nerve has died, then sensation may never come back to the area. Pain medication may be prescribed for less serious symptoms. Topical creams may also be tried to bring back sensation. Electrical nerve stimulation may be used for a period of time to stimulate nerves. Physical therapy can strengthen muscle and improve movement. Finally surgery might be necessary if pressure on the nerve is causing the neuropathy.
If you are experiencing sensation loss, numbness, tingling, or burning sensations in your feet, you may be experiencing neuropathy. Be sure to talk to a podiatrist to be diagnosed right away.
Walking on Uneven Surfaces While Hiking May Cause Blisters
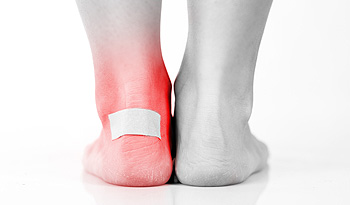 Many people enjoy hiking. Blisters can develop as a result of the miles that are walked on uneven surfaces, and they can be uncomfortable. Excessive friction is a reason blisters can form, which can be caused by wearing shoes and socks that do not fit correctly. A blister is defined as the body’s natural ability to heal damaged skin. A small bubble that is filled with protective fluid forms over the affected area, and will gradually drain as new skin forms. Research has indicated the importance of properly caring for your feet before beginning a hike. These methods can include treating an existing foot fungus, walking barefoot to toughen the skin, and keeping the toenails trimmed. If a blister develops, it can help to protect it with an elastic bandage while hiking is pursued. If you would like additional information about blisters, or if you have a blister that has become infected, please consult with a podiatrist.
Many people enjoy hiking. Blisters can develop as a result of the miles that are walked on uneven surfaces, and they can be uncomfortable. Excessive friction is a reason blisters can form, which can be caused by wearing shoes and socks that do not fit correctly. A blister is defined as the body’s natural ability to heal damaged skin. A small bubble that is filled with protective fluid forms over the affected area, and will gradually drain as new skin forms. Research has indicated the importance of properly caring for your feet before beginning a hike. These methods can include treating an existing foot fungus, walking barefoot to toughen the skin, and keeping the toenails trimmed. If a blister develops, it can help to protect it with an elastic bandage while hiking is pursued. If you would like additional information about blisters, or if you have a blister that has become infected, please consult with a podiatrist.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Dr. Scott Peters of Ankle & Foot Walk-In Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our office located in Mayfield Village, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.